I am really excited to unveil a new section of the website to you all today: An Additional Diagnosis Stories. A few months ago my friend Vicky, a Marf whom I look up to, came to me about the two of us creating a space to share information about what happens when people with Marfan syndrome and related disorders get another diagnosis, and how Marfan can affect the treatments for the new illness. I hope that this space will be able to serve as a good resource for patients and their medical team. Just as with the other sections, these guest posts will appear here and there on this blog, mixed in with everything else. We’ll start with Vicky’s story. You can view part two and part three here.
I have lived with Marfan syndrome for many years and I went through chemotherapy for breast cancer last spring. I realized that the treatment and experience of one condition affects the treatment and experience of the other. I hope we can share our thoughts and experiences of having an additional diagnosis, and learn together — as patients, and also as the medical providers who care for us. I’m hoping this will be a resource for patients and medical professionals alike. (I confess to being a medical professional. No wonder medical jargon constantly threatens to crowd out plain old lovely English.) I look forward to hearing from you.
I have a stark memory of a late afternoon phone call on the eve of Thanksgiving 1995. An abnormal mammogram, the doctor said — and, at age 41, my vision of myself as a woman with “just” Marfan syndrome abruptly changed. I was now a woman with Marfan syndrome and breast cancer.
It didn’t seem possible. Living carefully with Marfan, planning for upcoming aortic root surgery in the next six months to replace a growing aortic aneurysm (weakened bulge), I had felt somehow immune to another major diagnosis, as if my quota for managing life- threatening disease had been met. Now, another serious illness emerged. How would I cope? How would each condition influence my treatment options for the other?
When Marfan syndrome was untreatable, decades ago, few women with Marfan likely survived long enough to develop breast cancer (or enter menopause, for that matter). But since then, huge medical and surgical advances have dramatically improved the life expectancy in Marfan syndrome; now, many of us will live to a ripe old age. With increased years of life, though, we can also expect new health challenges, some due to Marfan, others completely unrelated — like breast cancer.
Marfan syndrome is relatively rare; unfortunately, breast cancer is not. One in eight women in the US will be diagnosed with breast cancer by the age of 90. So, as we Marfan women live longer, we might be increasingly likely to develop breast cancer – though I hope not one in eight of us. Maybe it will turn out that Marfan actually provides some protection against breast cancer, perhaps due to the Marfan tendency to have lower weight and body fat than the average American woman. This would be great news for us women who live with Marfan, but for now it’s only my wish, an untethered hypothesis.
All this is to say that I imagine I am not alone having Marfan and breast cancer. I am writing to share information, experiences and “musings” with others.
My medical team consists of a Marfan cardiologist, an oncologist and his nurse practitioner, and my primary care physician. I like them all. I am very lucky, for sure, because each is competent, kind and attentive, and each makes a unique contribution to my care. But none has ever seen Marfan with breast cancer before; we are all in this together, navigating uncharted territory. Thank goodness they are (for the most part) willing to listen to my Marfan point of view, and integrate it into their decisions for my
care. But sometimes I have felt resistance, disbelief, and skepticism. These times have been tough, and I have either felt discouraged, or more appropriately, had to fight harder to express my experiential knowledge of Marfan.
Here is an example.
While I was in chemotherapy earlier this year, I noticed that I had become short of breath. Any activity, walking across the living room, or even mashing ripe avocados for guacamole, would make me gasp for breath. It was very dramatic.
The oncology team noted around this time that the chemo drug had made me anemic, but it was apparently a mild anemia, so my marked breathlessness must be caused by something else. I was tested for other causes of shortness of breath, but no other explanation was identified.
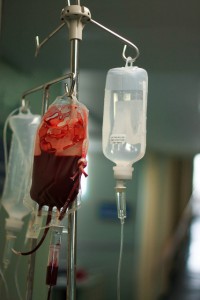
This was frustrating. I know from many surgeries over a lifetime how poorly my Marfan body adapts to anemia. But the oncology team was skeptical, and it took 3 months of my advocacy (pleading, really) before I received a blood transfusion. My symptoms were instantly relieved.
So, I learned that because I’ve had Marfan all my life, I needed to become a more pro- active teacher of all things Marfan. If my clinicians could keep an open mind, we would all master the Marfan-and-breast-cancer map together.
A little more about anemia in Marfan syndrome. (This is a bit technical, so bear with me here.) Shortness of breath is a common symptom. It can be traced to a variety of causes, including pulmonary embolism (blood clot to the lungs, which is more common in people with cancer); asthma; lung infection; edema (fluid buildup); and anemia. Usually, when someone is as breathless as I was, anemia is pronounced and often quite severe. But I had only mild anemia, with symptoms out of proportion to it in severity.
Why?
(Technical language alert continues.) There are two things about having Marfan syndrome that potentially could cause this disparity. Many of us with Marfan take beta- blockers. These curtail the body’s ability to raise the blood pressure and pulse, and give some protection to the aorta. In anemia, however, these medications could also theoretically blunt the body’s normal adaptive or compensatory mechanisms, making
the anemia “feel” more severe. The second possible explanation is the general aerobic deconditioning (being out of shape) that those of us with Marfan may experience. Deconditioned people, again, may not be able to compensate as well for anemia as others might. When considered together, in the same person with Marfan, perhaps these two effects are synergistic.
I really felt like a new person after that blood transfusion. And my frustration resolved when my oncologist finally understood how Marfan and anemia interacted in my case. I am not advocating serial/multiple blood transfusions to treat recurrent chemo-induced anemia. But, in a way, the transfusion was diagnostic – that is, it helped everyone understand the basis of my breathlessness so that the medical team could make decisions accordingly, now and in the future.
Are you a woman with Marfan syndrome and breast cancer? If you care to share your story, it would be a precious resource to others. In particular, how has having Marfan syndrome affected your choices and decisions for treatment of breast cancer?
Have you ever been diagnosed with anemia? What is your own experience of anemia in Marfan syndrome?
The opinions offered at Musings of a Marfan Mom are for informational purposes only and are not intended to be a substitute for professional medical advice, diagnosis or treatment. Always seek the advice of a qualified healthcare provider with any questions you may have regarding Marfan syndrome and any medical condition. Never disregard professional medical advice or delay in seeking care because of something you have read here.

4 Comments
Leave a reply →