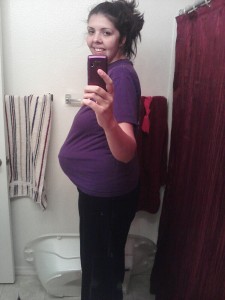
I’m now 31.5 weeks pregnant. It’s been a crazy past month, so I figured it’s time for another update. I started getting contractions somewhere around 26 weeks…I’ve lost track at this point. One day I realized I’d had them for 12 hours, so I asked Mark to take me to labor & delivery. My OB was out of town on a family emergency and the low-risk OB I saw didn’t know what to do about me since the typical tests all looked fine. He decided to just send me home, without any medication even, and told me to stay off my feet the rest of the week.
The contractions didn’t stop; the next day, 36 hours after they’d started, Mark drove me to the high-risk clinic. I talked to the nurse and insisted on seeing a high-risk resident. Long story short, I was harassed by one of the nurses (who knew NOTHING about Marfan) and again sent home. No one would contact my OB and I felt like I shouldn’t because he was out of town. My cardiologist was also gone. It took almost a week before the contractions stopped without me being flat on my back. They continued to come off and on, always painfully.
I don’t remember how many L&D/hospital trips I’ve made this pregnancy, but with each trip I’ve grown increasingly frustrated.
So, last weekend was our Marfan chapter’s annual BBQ and I had a chance to talk with my cardiologist. I laid out everything I was upset about: no real contact with high-risk OBs, general lack of Marfan knowledge, no one listening to me. For instance, why was one doctor advocating weekly Non-Stress Tests (NSTs) but not ultrasounds of my cervix to check for shortening? Why not stop the contractions with progesterone instead of risk them beginning to dilate me, since Marfan already puts me at risk for pre-term labor? I was not expecting my cardiologist’s suggestion that if I wasn’t happy, I consider switching to another OB, one he used to work with, at another hospital in another city. I had never considered that to be an option.
This week I met with my OB for the first time in over a month. I laid everything out for him (except that Mark and I have been considering changing hospitals). I appreciated his honesty, but I’m dismayed at some of the information that I got.
For starters, I will be delivered by a low-risk OB, not an MFM. MFMs do not deliver babies vaginally apparently (just scheduled c-sections). Unlike smaller hospitals, there is a full obstetric staff available 24 hours a day so I won’t have to wait for an OB or anesthesiologist to come in from home when the baby is ready to be born, so that’s great, but the MFMs do not stay at the hospital and only come in if there is a major emergency, though they are available for questions over the phone. I had been under the impression since our pre-conception appt. that when my OB had said he “probably” wouldn’t be delivering my baby, he meant there would be a 1 in 6 or 8 chance that he would; that whichever MFM was on call that night would be delivering me, NOT that the only way he would is if I scheduled a c-section with him.
He’s also insisting on me having weekly NSTs. I disagree that they’re so necessary, but I said I would go if he would first deal with the nurse who harassed me last time. I watched him take names and notes so I do trust that he’ll follow up on it. Apparently at 32 weeks cervical ultrasounds stop being so accurate but he said he’ll do manual checks at each visit from now on if I want them.
On the upside, he promised no pitocin induction for me. IF down the road I am very dilated and effaced I can elect for him to strip my membranes, which I doubt I will, but that’s it. My OB also assured me that my VBAC plans are all over my chart.
So here’s my big question. If I’m SOOOO high risk that I need an MFM, one who specializes in my genetic disorder, and I need special delivery plans with meetings with multiple specialities every trimester, then why I am I suddenly ok to deliver with any old OB at the hospital? That’s when I am MOST at risk for dissection. I do not like this. I do not trust they will believe me if I have a dissection. I know it’s a different hospital this time around, but I am still angry over how I was treated when I had Menininho, how none of the doctors or nurses listened to me when I was sick, and so I don’t trust anyone.
But, when Mark and I outlined all the costs and benefits of switching hospitals, we decided I should stay where I am. The other hospital is up to 3 hours away, depending on traffic. Since I’ve not had labor before, I have no idea how fast I might deliver and I do not want to risk being in hard labor or, heaven forbid, dissecting while stuck in traffic. Plus, it’s really far to drive for weekly appointments in general. No one at the hospital will know me or my medical history, unlike my cardiac team at Stanford, whom I trust with everything. I’d also need to get a new doula, and I really am attached to my current one.
I forsee more conversations with my OB and cardiologist in my future, really serious ones about ensuring I will be taken care of. The one upside I can think of though, is that perhaps delivering with a low-risk OB, the doc will be more flexible with when I get my epidural and IV, since it’s not like they’ve been very conservative about anything so far.

12 Comments
Leave a reply →